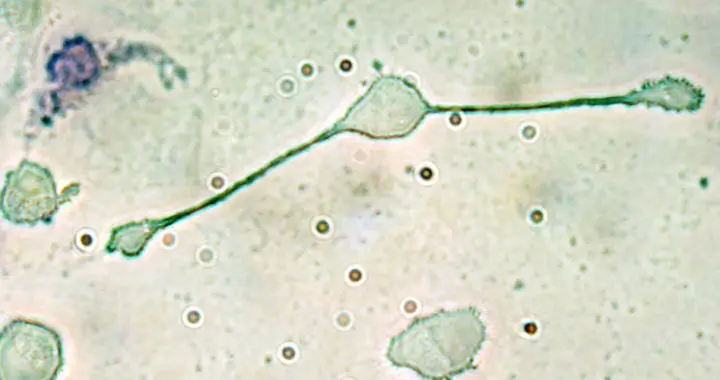
Macrophages are one of the major types of white blood cells or leukocytes of the immune system that play an important role in the innate immune response against pathogens, foreign substances, cancer cells, and cellular debris.
What Are Macrophages? Where Do They Come From? How Do They Work?
Origins and Development of Macrophages
Some of these cells are seeded early in the embryo and then maintained throughout adult life. However, most originate from monocytes circulating in the blood. Note that monocytes are another type of leukocyte capable of differentiating into either macrophages or dendritic cells. They originate in the bone marrow from precursor or progenitor cells called monoblasts.
These monocytes circulate in the bloodstream for one to three days before moving into tissues to differentiate into macrophages and dendritic cells. They also moved to damaged tissues or sites of infection through a process called leukocyte extraversion and chemotaxis. Hence, upon their arrival to an area that requires an immune response, monocytes differentiate into macrophages.
It is also important to highlight the fact that different stimuli attract the migration of more monocytes to a particular area. These include damaged cells, cellular debris, presence of pathogens and their pathogenic activity, and the release of cytokines by macrophages already present in the damaged tissue or site of infection.
Specific Roles or Functions of Macrophages
Understanding the role of macrophages in the immune system first requires an understanding of their different classifications based on their fundamental functions and activation. Note that these cells differentiate further to specific population groups with specific roles. The process is called macrophage polarization. Below are the three broad functional classifications or groupings of macrophage population:
1. Classically Activated
Classically activated macrophages or M1 are activated via the stimulation of specific interferons, chemokines, and molecules called lipopolysaccharides and lipoteichoic acid.
Note that interferons are secreted by host cells infected by a virus, while lipopolysaccharides are found in the outer membrane of gram-negative bacteria and lipoteichoic acid on the cell wall of gram-positive bacteria.
M1 can also be activated via a glycoprotein called granulocyte-macrophage colony-stimulating factor. Existing macrophages in an area and other leukocytes such as thymus lymphocyte or T cells release this substance in response to an infection,
The primary role of M1 is to kill host cells infected by a virus or haunt and kill bacteria. They specifically engulf and digest infected cells and pathogens. M1 also produces chemicals called reactive oxygen species and nitrogen radicals to enhance their ability to kill pathogens.
M1 cells are also pro-inflammatory immune cells. They release pro-inflammatory cytokines to attract and recruit more macrophages and other immune cells to the target area.
2. Alternatively Activated
Remember that M1 cells are primarily antimicrobial and pro-inflammatory macrophages. On the other hand, alternatively activated macrophages or M2 have opposite functions.
The primary roles of M2 cells are to promote extracellular matrix construction, the proliferation of cells, and angiogenesis or the formation of new blood vessels. In contrast, M1 promotes extracellular matrix destruction, apoptosis, and inflammation.
Activation of these cells transpires through the release of anti-inflammatory cytokines such as interleukin 3, interleukin 4, and interleukin 10, as well as by the specific biological condition, the presence of prostaglandins, and apoptosis or programmed cell death.
It is important to stress the fact that M2 cells are fundamental in tissue repair and wound healing. Hence, they are also called wound-healing macrophages.
3. Regulatory Macrophages
Another functional category represents so-called regulatory macrophages or Mregs. Some group them under the M2 classification while others insist a separate grouping. They also closely resemble M1 cells than M2 cells.
Nonetheless, Mregs have the primary function of regulating the immune response by dampening inflammation and limiting immunopathology. They are activated following either innate or adaptive immune response.
The exact cause of how macrophages differentiate further to Mregs remains unknown. Current assumptions behind their molecular mechanism include activation via the extracellular signal regulated kinase and ligation of the Fc receptor.
When compared to M1, these cells produce high levels of anti-inflammatory cytokines such as interleukin 10 and hampers the synthesis of the pro-inflammatory interleukin 11 cytokines. They also do not contribute to the construction of extracellular matrix, unlike M2.
Specific Rundown of Functions and Significance
Aside from the aforementioned functional categories, the following is a summary of the different roles or functions of macrophages:
• Innate Immune Response: Remember that they are one of the frontliners of the innate immune system. They are phagocytes capable of phagocytosis that involves the engulfing and digestion of pathogens, cellular debris, foreign substances, and cancerous cells.
• Role in Adaptive Immunity: They digest a pathogen and integrate its antigen to their structure to present to the helper T cells. These helper T cells would then promote the activation of other macrophages and cytotoxic T cells.
• Immunoregulation: These cells also regulate the immune system and the immune response. Remember that M1 cells are responsible for pro-inflammatory mechanisms while M2 and Mregs have anti-inflammatory functions.
• Healing and Regeneration: Increased muscle use leads to minuscule tissue damages and inflammation. M2 oversees muscle repair and growth. M1 is responsible for clearing a wounded site of pathogens and cellular debris. M2 initiates wound healing.
• Tissue Homeostasis: Non-migratory macrophages residing in tissues provide growth factors to support their normal physiological functions, while also actively protecting them from inflammatory damages.
Despite the important role of macrophages in the immune system and the body, they have also been implicated in numerous diseases and conditions. For example, they are common host cells for several intracellular pathogens such as the Mycobacterium tuberculosis, Leishmania parasite, Chikungunya virus, and human immunodeficiency virus, among others.
They can also contribute to the proliferation of cancer cells and tumor growth by fostering tumor angiogenesis and suppressing antitumor leukocytes. Specifically, because they are naturally attracted to oxygen-starved and necrotic tumor cells, they promote chronic inflammation and other immune responses that could support the proliferation of malignant cells.
Studies have also observed that high numbers of pro-inflammatory macrophages within the adipose tissue of a clinically obese individual result in obesity complications such as insulin resistance and type 2 diabetes. Fat cells in obese tissues are predisposed to necrotic death that prompts resident M2 cells to switch to the pro-inflammatory M1 phenotype. Photo credit: Obli/Adapted/CC BY-SA 2.0
FURTHER READINGS AND REFERENCES
- Fairweather, D. and Cihakova, D. 2009. “Alternatively Activated Macrophages in Infection and Autoimmunity.” Journal of Autoimmunity. 33(3-4): 222-230. DOI: 1016/j.jaut.2009.09.012
- Murray, P. J. 2017. “Macrophage Polarization.” Annual Review of Physiology, 79(1): 541-566. DOI: 1146/annurev-physiol-022516-034339
- Orecchioni, M., Ghosheh, Y., Pramod, A. B., and Ley, K. 2019. “Macrophage Polarization: Different Gene Signatures in M1(LPS+) vs. Classically and M2(LPS–) vs. Alternatively Activated Macrophages.” Frontiers in Immunology. 10. DOI: 3389/fimmu.2019.01084
- Wynn, T. A., Chawla, A., and Pollard, J. W. 2013. “Macrophage Biology in Development, Homeostasis, and Disease.” Nature. 496(7446): 445-455. DOI: 1038/nature12034